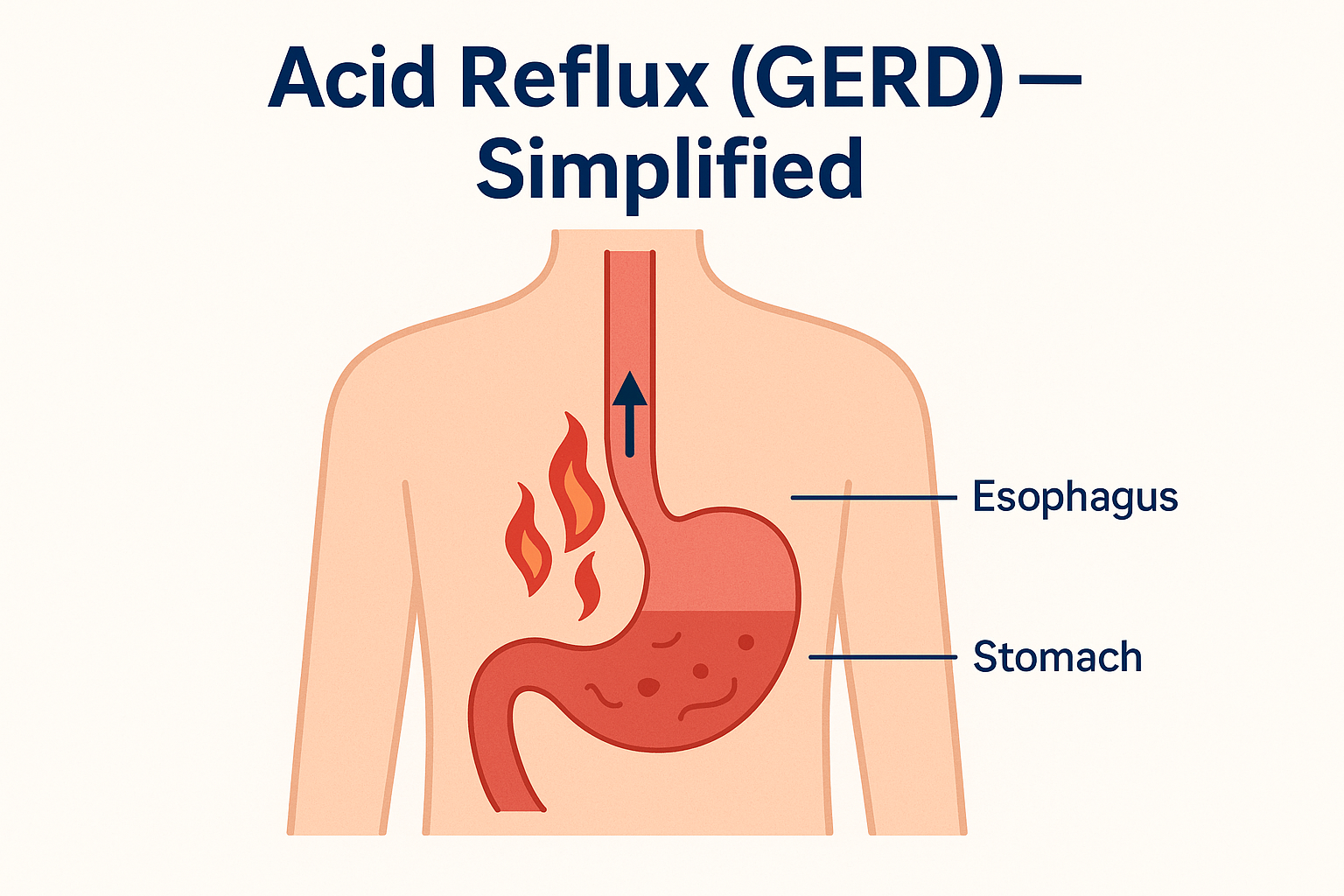
What Is Acid Reflux?
Acid reflux happens when stomach acid flows back into the esophagus — the tube that connects your mouth to your stomach.
The stomach is built to handle acid… the esophagus is not.
When the valve between them weakens, acid escapes and causes irritation.
Common Symptoms
- Burning in the chest (heartburn)
- Sour or bitter taste in the mouth
- Food or liquid coming back up
- Chronic cough or throat clearing
- Hoarseness
- Chest discomfort after meals or lying down
Why Acid Reflux Happens
Food triggers
- Spicy foods
- Coffee
- Chocolate
- Fatty meals
- Citrus
- Tomatoes
- Mint
Lifestyle
- Eating late at night
- Large, heavy meals
- Lying flat after eating
- Smoking
- Obesity
Medical
- Pregnancy
- Hiatal hernia
- Certain medications (NSAIDs, some BP meds)
When Is It GERD?
Reflux becomes GERD when:
- Symptoms happen 2+ times per week
- They impact daily life
- There is esophageal irritation or inflammation
Lifestyle Changes That Actually Work
- Stop eating 2–3 hours before bed
- Eat smaller meals
- Elevate the head of the bed
- Identify and reduce food triggers
- Lose weight if needed
- Stop smoking
Medications
Antacids
Quick relief (Tums, Gaviscon)
H2 Blockers
Short-term acid control (Famotidine)
PPIs — Most Effective
Examples:
Omeprazole, Pantoprazole, Esomeprazole
Used once or twice daily depending on severity.
When to See a Doctor
Seek medical care if you have:
- Difficulty swallowing
- Food getting stuck
- GI bleeding (vomiting blood, black stools)
- Unexplained weight loss
- Persistent symptoms despite medications
These could indicate complications like esophagitis or Barrett’s esophagus.
Takeaway
Most patients improve with:
- Consistent lifestyle changes
- Identifying triggers
- Proper use of medications
If symptoms persist, an upper endoscopy (EGD) may be needed to check for irritation or complications.